Hypertrophic Cardiomyopathy (HCM)
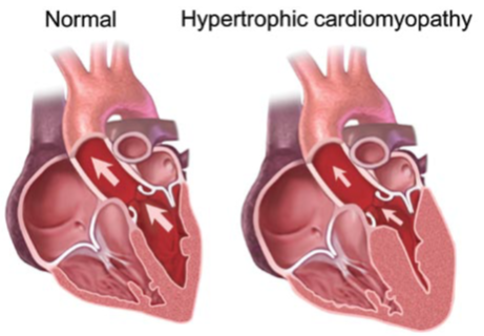
Hypertrophic cardiomyopathy (HCM) is the most common heritable cardiac condition and is the most common cause of sudden cardiac arrest in the young, affecting about 1 in 500 people. Familial hypertrophic cardiomyopathy is a heart condition characterized by thickening (hypertrophy) of the heart muscle, more specifically the ventricle. The thickened heart muscle, can make it challenging to keep up with the oxygenation demands of the body and the heart muscle itself. Many people with HCM have few, if any, symptoms and can lead normal lives without significant symptoms. However, this condition can also have serious consequences. Life threatening arrhythmias resulting in cardiac arrest can sometimes be the first symptom.
Signs and symptoms of hypertrophic cardiomyopathy may include one or more of the following:
- Shortness of breath, especially during exercise
- Chest pain, especially during exercise
- Fainting, especially during or just after exercise or exertion
- Sensation of rapid, fluttering or pounding heartbeats (palpitations)
- Heart murmur, which a doctor might detect while listening to your heart
Treatment and Management:
Managing hypertrophic cardiomyopathy requires lifelong annual visits with a cardiologist to screen for potential cardiac risks and obtain a careful family history. Routine testing can consist of echocardiograms, 12 lead ECG, Holter monitoring, exercise stress test, cardiac MRI, or a blood test for cardiac genetic testing.
Common information that may be attained from the tests?
Echocardiogram (Echo): The structure and function of the heart. The degree of thickening and shape of thickened area. Is the thickened area creating an obstruction to the (aorta) artery that supplies oxygenated blood to the body? Is there any mitral valve involvement or regurgitation? If the patient has a transvenous lead from implanted hardware, how is this lead impacting the structures within the heart?
12 lead ECG: Reveals the baseline rhythm, if the patient is paced, the function of the device. The voltage force of the ventricle and the recovery of the heart muscle.
Holter: Rhythm throughout the monitored period, any evidence of arrhythmias
Exercise Stress Test: any evidence of ischemia (decreased oxygenation to the heart muscle), any inducible arrhythmias throughout the test or in the post exercise period, and blood pressure response during exercise.
Cardiac MRI: measurements of the ventricle chamber size, degree of hypertrophy, areas of scar.
Genetic testing: blood test that extracts DNA that is analyzed to identify mutations in the genes that are associated with HCM. This test is resulted as a positive, negative, or a variant of uncertain significance.
There are multiple reasons why genetic testing may be recommended:
- This may help your provider in some cases if the diagnosis itself is not clear with clinical data alone, like in the case of an athlete’s heart.
- Once a gene mutation is identified, cascade testing can be performed in first degree relatives.
- Knowledge of the disease causing gene will foster informed family planning decisions.
- There are also instances where the individual may be asymptomatic with no positive clinical findings other than the positive gene mutation.
A positive test result confirms the diagnosis of HCM. A negative result indicates that a disease causing mutation associated with HCM was not identified. Importantly, this does not rule out the possibility of having the disease, but that a disease causing mutation has not been recognized yet on the HCM panel. A variant of uncertain significance is an inconclusive finding of a DNA abnormality, and is unclear if the change can cause HCM. The genetic test results will be discussed with you by your medical team and may also be discussed by a genetic counselor.
Common treatment recommendations are cardiac medications to decrease the heart rate and improve the filling time between heartbeats. Other treatments may be a surgical myectomy to decrease the amount of obstruction from the aorta (the vessel that supplies oxygenated blood to the body). For rhythm management and protection from a life threating rhythm problem an implantable cardiodefibrillator (ICD) may be warranted. A small number of affected patients can develop heart failure and require heart transplantation.
