Wolff-Parkinson-White Syndrome (WPW)
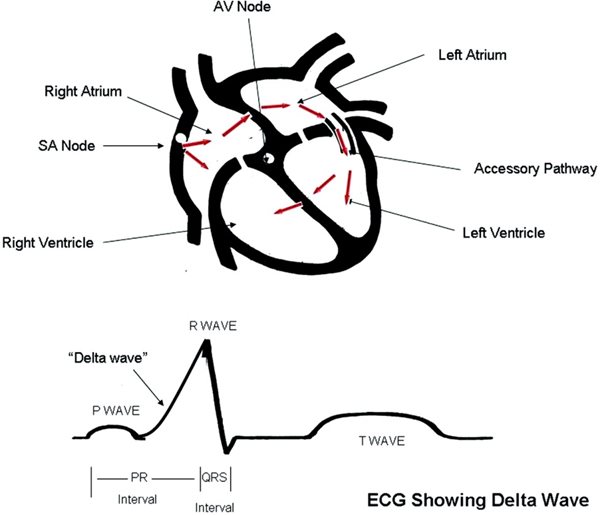
Wolff-Parkinson-White (WPW) syndrome is an abnormality of the heart's electrical conduction system which can be associated with supraventricular tachycardia (SVT). In WPW syndrome, there is an extra electrical pathway (called an "accessory pathway") in the heart which can transmit electrical impulses from the upper chambers (atria) to the lower chambers (ventricles) of the heart. In the normal conduction system, there is only one electrical conduction pathway from the atria to the ventricles. It is called the atrio-ventricular node (AV node). A WPW pathway bypasses the AV node and can transmit electrical signals through the heart faster than through the AV node This can cause SVT or other abnormal heart rhythms.
When impulses travel from the atria to the ventricles through the extra pathway, the ECG shows a pattern called a Delta wave or "pre-excitation". Each patient is different in how fast electrical impulses can be transmitted over this pathway. If the pathway is able to transmit very fast and if the patient has an arrhythmia known as atrial fibrillation (in which the atria pump from 300-600 times/minute), the extra pathway may transmit that very rapid rate.
Signs and Symptoms
Symptoms of Wolff-Parkinson-White syndrome are the result of a fast heart rate. Common symptoms of WPW syndrome include:
- Sensation of rapid, fluttering or pounding heartbeats (palpitations)
- Dizziness
- Chest discomfort
- Difficulty breathing
- Lightheadedness
- Tiring easily during exercise
- Anxiety
An episode of a very fast heartbeat can begin suddenly and last for a few seconds or even as long as several hours. Episodes often happen during exercise, but may also occur during quiet activities.
Some people with Wolff-Parkinson-White syndrome occasionally experience a type of irregular heartbeat known as atrial fibrillation. In these people WPW signs and symptoms may also include:
- Chest pain
- Chest tightness
- Difficulty breathing
- Fainting
- Rarely, sudden death
Symptoms in infants with Wolff-Parkinson-White syndrome may include:
- Rapid or labored breathing
- Lack of alertness or activity
- Poor eating
- Fast heartbeats visible on the chest
Most people who have an extra electrical pathway in the heart experience no fast heartbeat and no symptoms. This condition, called "Wolff-Parkinson-White pattern", is usually discovered by chance when a person is undergoing a heart exam for other reasons. Wolff-Parkinson-White pattern is harmless in many people. But doctors may recommend further evaluation before children with WPW pattern participate in high-intensity sports.
Diagnosis
WPW is discovered on the ECG (electrocardiogram). Information on ECGs are in the basic Electrophysiology fact sheet.
Some patients find out they have WPW because they had an ECG for another reason not related to their heart, such as a sports physical. Some patients are diagnosed after having an episode of SVT. The heart in patients with WPW may be built normally, or may be associated with structural abnormalities.
Finally, some patients find out they have WPW when they are admitted through the emergency department after having an episode of fainting or in rare occasions after cardiac arrest.
Treatment
Treatment may include medication to prevent SVT. In babies, medication is given to prevent SVT for the first year. Up to 2/3 of babies will "outgrow" WPW when diagnosed at an early age (in the first year of life) and will not require further treatment.
The best way to determine if a patient is at risk for sudden death from their WPW pathway is an EP study.
Cardiac (heart) ablation has become the first line of treatment in older patients, especially in older children or adults.
Lifestyle Changes:
Until a patient’s WPW has been fully evaluated, patients may have some restrictions on vigorous exercise, which is determined by the electrophysiologist or cardiologist caring for the patient.
Typically, if the extra pathway in WPW does not transmit very rapidly, then the patient does not have activity restrictions.
If a patient has a high-risk pathway that has not been ablated, he or she may be restricted from strenuous activities.
